For routine visits, emergencies, and general enquiries
Get Direction
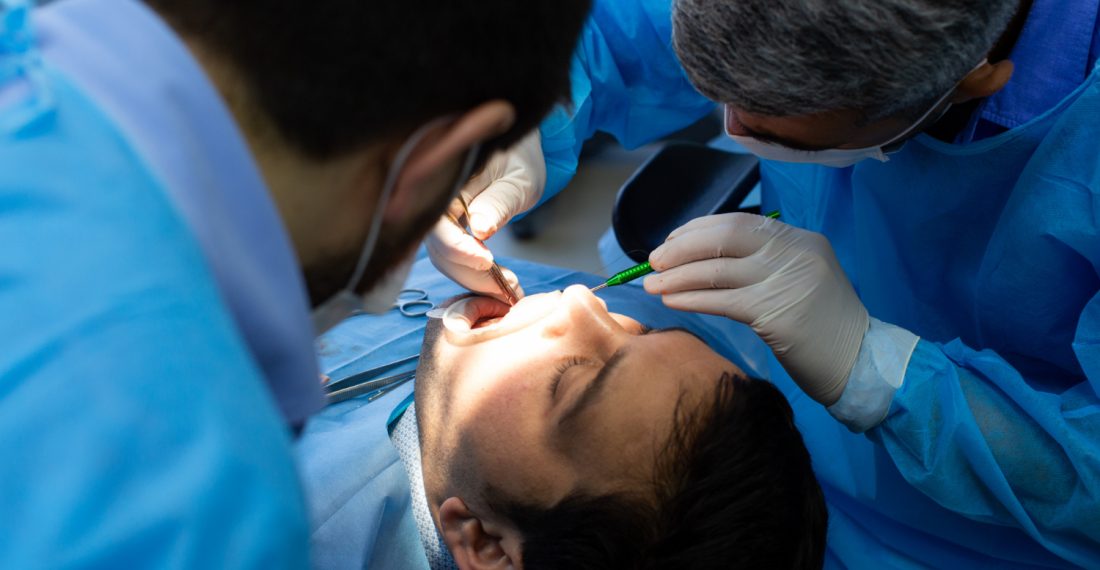
Root canal is a part of endodontics, which in turn is a part of dentistry focusing on the innermost part of a tooth, its pulp and roots. Root canal specialises in procedures done to remove infection and save the tooth from permanent damage and pain. Now, because this procedure involves handling the tooth’s pulp where blood vessels and nerves reside, people expect a lot of pain both during and after this treatment, making it an anxiety inducing topic in a dental clinic.
If your dentist has mentioned a root canal, you might be reminded of all the horror stories you’ve come across both online and in person. Modern root canal treatment, also known as RCT, is one of the most misunderstood procedures in dentistry while being one of the most effective ones instead. This guide filters through the noise, answering the questions you’re actually worried about and giving you clinically backed information that will help to better understand the procedure before making any decisions.
Your tooth is made up of more than just the hard white surface you brush every day. Inside every tooth lies a soft tissue called the pulp, which are nerves, blood vessels, and connective tissue all bundled together. When this pulp becomes infected or inflamed, it can no longer heal itself, and poses a risk to the other layers of your teeth and your gums. This is when a root canal, or endodontic treatment, becomes necessary.
Signs you may need root canal treatment include:
It’s worth noting that an infected tooth can have no obvious pain at all in the case where its internal nerves may already be dead. This is why regular dental check-ups and X-rays are irreplaceable; they allow your dentist to catch pulp disease before it escalates into something far more difficult and costly to treat.
If you’re experiencing any of the above, do not delay. The longer an infection is left untreated, the more time it has to keep spreading, which in the worst case can lead to life-threatening complications.
To address the most common question head-on about root canal pain, the answer is no, not really. Whatever discomfort you’ve been enduring before the procedure is more than likely to be worse than anything you will have to endure during and after your RCT.
The notorious reputation of root canal pain is a lingering remnant from a bygone era of dentistry. Today, the procedure is performed under local anaesthesia, which fully numbs the affected tooth and surrounding area. Most patients report feeling nothing more than a mildly pressurised sensation during treatment. Some even fall asleep.
People often get misled by the pre-treatment throbbing agony of an infected tooth, with the procedure itself. What you need to know is that root canal procedures don’t cause your pain. They end it. Within days of treatment, the agonising pressure from the pulp and infection-driven nerve irritation should be gone.
While some mild soreness and sensitivity near your tooth can linger for a few days after the procedure, it is easily managed with easily prescribed painkillers like ibuprofen or paracetamol. Most patients feel entirely normal within one to three days, with recovering fully typically within the first week.
Dental anxiety is far more common than most people admit. Even for people who don’t show it, the thought of sitting in the dentist’s chair for a seemingly invasive procedure can genuinely be a cause for distress. If you are feeling the same, please know that you are not alone, and a good endodontic practitioner will acknowledge that and use methods that help to calm such feelings. Warner Dental’s dedicated dental anxiety and phobia support service is designed specifically with these cases in mind.
The treatment’s clinical approach begins with understanding your specific triggers and medical history before any treatment is discussed. Zero pressure to rush straight to the treatment chair. For patients who need support beyond reassurance, structured sedation options are assessed on an individual basis:
Administered in-clinic, focused on rapid effectiveness and recovery. You remain conscious and responsive throughout, making it ideal for mild to moderate anxiety. This is the most commonly used option for nervous patients undergoing root canal treatment at Warner Dental.
A prescribed sedative taken before the appointment that induces a deeply relaxed, drowsy state. As long as you meet the eligibility from your medical history and have someone to escort you home, your full procedure can be completed with minimal distress.
For severe dental phobia or particularly complex cases, IV sedation is administered by a qualified Anaesthetist. You remain conscious but in a deeply calm state, with little to no memory of the procedure afterwards. Recovery time can be longer, and an escort is required for your safety.
Every appointment at Warner Dental uses consent-based, step-by-step care. You can pause or stop at any time. This ability alone significantly reduces the perceived threat of the treatment, as it reduces the feeling of powerlessness.
As for the duration of the RCT, a straightforward front tooth root canal can take as little as 60 to 90 minutes in a single appointment. For Molars which have multiple roots and more complex canal structure, a total of two visits of 90 minutes each can sometimes be necessary. Your root canal dentist will give you a realistic timeline based on which tooth is involved and the complexity of the case before beginning the treatment. Knowing that the procedures don’t even take that long should also be a step in boosting one’s confidence.
One of the biggest improvements in modern endodontic treatment is how genuinely impressive the technology used during said treatment has become over the ages.
Cone Beam Computed Tomography (CBCT): Unlike traditional 2D dental X-rays, CBCT imaging provides a full 3D view of the tooth and surrounding bone. This allows your root canal dentist to map every canal precisely to detect curved, narrow, or calcified canals that would otherwise go undetected, all before a single RCT cleaning tool reaches near your face.
Dental Operating Microscopes: Specialist endodontists routinely use high-powered microscopes that can magnify their vision by up to 25 times. This level of precision significantly improves the thoroughness of canal cleaning and filling.
Nickel-Titanium (NiTi) Rotary Instruments: These ultra-flexible instruments navigate the curved anatomy of roots far more effectively than the old stainless-steel hand files. They’re faster, more precise, and gentler on the tooth structure.
Electronic Apex Locators: These devices accurately determine the exact length of the root canal in real time, eliminating guesswork and reducing the chances of over-cleaning or missed spots.
Ultrasonic Irrigation Systems: After the canals are shaped, they must be thoroughly disinfected. Ultrasonic activation of residual irrigants improves the removal of bacteria, biofilm, and debris from areas that instruments or even liquid may find difficult to reach.
In combination, this technology has transformed what was once a difficult, multi-visit ordeal into a precise, predictable, and often single-appointment procedure.
If you’ve spent any time researching root canals online, you may have come across alarming claims about their safety, which may include documentaries or theories suggesting root-canal-treated teeth being the cause for cancer, heart disease, or arthritis.
These claims trace back to a research conducted in the 1920s by Dr. Weston A. Price, whose research suggested that bacteria trapped in the tiny tubules of a root-filled tooth could leak into the bloodstream and cause many diseases. While it sounds alarming, we must realise that it was also conducted over 100 years ago, that too using methods that would fail almost each and every standard that our modern clinical practices are guaranteed to meet.
Conversely, newer evidence supports successful RCTs to have a beneficial impact on our health as it reduces the burden that our body would need to face had the infected tooth been left untreated. In other words, treating the infected tooth is what protects your overall health.
The cost for a root canal is ultimately the main factor in whether or not you move forward with undergoing the treatment, and understandably so.
In Australia, dental treatment needs to be funded by oneself in the case for most adults, as Medicare generally does not cover routine dental services. This means the price that you pay depends on the type of infected tooth and the complexity of its case. At Warner Dental, all costs are discussed and documented in a written treatment plan to ensure there are no surprises.
The single biggest cost variable is the tooth being treated. Front teeth (incisors and canines) typically have a single, straight root canal and are the quickest to treat. Premolars have one or two canals. Molars are the most complex as they can have three or more canals with curved anatomy, which requires more time and precision. As a general reference, root canal costs across Australia range from approximately $800 to $1,200 for front teeth, and $1,500 to $2,500 or more for molars, depending on the procedure’s complexity. If a dental crown is recommended to protect the tooth after treatment, which is common for back teeth, its cost will also be mentioned upfront by your dentist during your initial consultation.
If you hold extras or ancillary dental cover, your health fund will typically contribute a rebate toward root canal treatment, reducing your out-of-pocket costs. Warner Dental is a preferred provider for NIB, HCF, and CBHS, and accepts all major health funds via HICAPS on-the-spot claiming, meaning your rebate is processed immediately at the time of your appointment, so you only ever have to pay the difference. Funds accepted include Bupa, Medibank Private, Australian Unity, Teachers Health, and many more. Contact us to determine your level of covered costs before your appointment.
The key takeaway that you should keep in mind is: cost should not be a reason to delay treatment that can save one’s natural tooth. Between health fund rebates, government programs, and flexible payment plans, Warner Dental has multiple pathways to make root canal procedures more financially accessible. Furthermore, our team will walk you through every available option before you make up your mind to commit to any specific treatment plan.
The topic on cost is incomplete without talking about how long you can actually enjoy the benefits of your investment.
Long-term data from a study conducted in 2023 shows cumulative survival rates of teeth that have undergone root canal as 97% after 10 years, 81% after 20 years, 76% after 30 years, and 68% after 37 years for endodontically treated teeth. That’s not a temporary fix — that’s decades of function from a tooth that would otherwise have been lost.
One critical factor that can have significant influences on these outcomes is the quality of the restoration done to your tooth after the root canal. A good-quality coronal restoration is necessary to completely heal your tooth. Dental seals for the visible parts of your teeth are found to be as important as the quality of the endodontic treatment itself in terms of treatment success. Simply said, have your dentist seal the site of the root canal meticulously using dental caps, or any other recommendation.
With these measures in place, a root canal-treated tooth can last for a long time.
Many patients are tempted to skip the root canal and simply extract the tooth as it seems cheaper and more decisive. But this thinking rarely accounts for the full picture.
When a tooth is extracted, the gap it leaves can create a cascade of biological consequences. Adjacent teeth begin to drift into the empty space over time. The opposing tooth, no longer meeting its partner, can grow downward or upward, getting out of position. The jawbone in the extraction area begins to shrink within months, changing facial contour and making future restorative work more complicated.
To properly replace an extracted tooth, you would be looking at:
None of these options replicate the feel, function, or biomechanics of your natural tooth. And every one of them costs significantly more than a root canal and crown combined in the long term, without delivering a superior result. An extraction may feel like an easy exit today, but it can often become a far more expensive and complex problem within five to ten years.
Not all root canal treatment is equal. For straightforward cases on front teeth, a well-trained general dentist is perfectly capable. For complex cases involving heavily curved roots, calcified canals, previous failed treatment, or molar teeth with multiple roots, a specialist endodontist makes a meaningful difference.
Endodontists complete three to four years of additional full-time postgraduate training on top of their general dentistry degree, being able to specialise in the diagnosis and treatment of pulpal disease. They work with advanced tools and imaging as a standard, not an upgrade.
Root canal treatment has a reputation it does not deserve. It is a safe and effective procedure, and in the vast majority of cases, it is the best possible solution for a tooth that has been compromised by infection or pulp damage. Modern techniques, materials, and equipment have made the procedure more comfortable and more consistent than ever before in dental history.
The only feeling worse than needing a root canal is facing the consequences of avoiding one. An untreated infection doesn’t simply go away, it spreads. And a tooth that could have been saved for decades of use turns into one with the ability to take more of your teeth to follow it on its eventual way out. Ultimately, this outcome bears a far greater cost to your health, comfort, and your finances.
If your dentist has recommended an RCT, get your worries answered, your total bill quoted, and take the appointment.
Mild throbbing after treatment is normal. It signals your body’s inflammatory response settling down around the recently treated area.
During root canal treatment, your infected pulp tissue is removed and the canals are cleaned and sealed. The surrounding ligament and bone go through a short-term inflammatory response as they begin to heal. This feeling typically peaks within 24 and 48 hours and gradually improves. After a root canal procedure, some mild pain or discomfort is expected and usually resolves quickly. Persistent or worsening pain beyond a week warrants review.
Avoid chewing on the treated side until your final restoration is placed. Over-the-counter ibuprofen or paracetamol can manage post-treatment discomfort well until a certain level, but another dental consultation is recommended if the pain is unnaturally strong or lasts much more than two days.
No. If you have received oral sedation or IV sedation, you will be unable to drive for a prolonged period. Please arrange a responsible adult as your escort.
Being sedated will significantly impair your coordination, judgment, and reaction time even when you feel you have recovered. Queensland Patient information on anaesthesia confirms that sedation affects judgment for up to 24 hours or longer. Happy gas (nitrous oxide) clears the system quickly, and most patients can drive after a short recovery period — but your dentist will confirm this individually. For any other form of sedation, driving is not permitted on the day of treatment.
Book your driver before your appointment, not after. Avoid relying on rideshare as a substitute for a trustworthy and responsible escort.
Without a crown, your treated tooth is vulnerable to fracture, reinfection, and structural failure, especially the molars.
A root canal-treated tooth has had its internal pulp removed, leaving it temporarily more brittle than a living tooth. The Victorian Government’s Better Health Channel notes that teeth requiring root canal treatment have often already lost significant tooth structure and may require further protection in the form of a crown. Without one, the tooth can crack under normal chewing forces, and bacteria from the mouth can leak back in through any microscopic cracks, undoing the treatment entirely. While your front teeth do carry a lower risk for fracture and may be restored with a filling alone, your back teeth almost always require a crown.
Have your crown placed as soon as your dentist recommends. Delaying this step is the most common reason a successful root canal ultimately fails.
With proper restoration and oral hygiene, a root canal-treated tooth can last decades.
Long-term clinical data shows cumulative survival rates of 97% at 10 years, declining gradually to 68% at 37 years of follow-up. This means the majority of treated teeth remain functional well into a patient’s later life. The Victorian Government’s Better Health Channel confirms that about 90 to 95% of patients can expect a functional tooth after treatment, given that oral hygiene is maintained. The quality of the crown or filling placed after treatment, and whether the patient wears a night guard if they grind are the two most significant factors influencing long-term survival.
Attend your six-monthly check-ups. Your dentist will monitor the treated tooth with periodic X-rays to catch any early changes before they can become a problem.
Yes. Root canal treatment is safe for children and is often recommended to preserve both baby and permanent teeth.
For baby teeth with infected pulps, a procedure called a pulpotomy, which is a general form of a partial root canal is done as the standard treatment. Queensland Health’s patient information confirms pulpotomies have a high success rate and are performed under local anaesthetic, with a crown placed afterwards to protect the tooth. Preserving infected baby teeth matters: Better Health Channel confirms that baby teeth lost too early allow adjacent teeth to drift and disrupt the path of incoming adult teeth. For children with permanent teeth already erupted, standard root canal procedures are performed using the same protocol as adults.
If your child has a toothache or facial swelling, seek dental assessment promptly. Early treatment avoids the need for more complex procedures and protects the developing adult dentition.